In a highly prominent position in Canadian healthcare stands the Jewish General Hospital (JGH). Dr. Lawrence Rosenberg, President and CEO of the organization, walks us through the JGH’s experiences over the past two years, with an update on the hospital’s latest developments.
INTRODUCTION
The healthcare services and technology sector has acquired added importance over the past two years, as global businesses and organizations have worked with exceptional intensity to weather the COVID-19 pandemic and improve the lives of the people in the communities they serve.
Based in Montreal, the Jewish General Hospital (JGH) is one such entity. With a proud history of helping those in need of medical attention, the JGH was one of the first of two adult hospital centers designated by the Government of Quebec to receive COVID-19 patients.
“The JGH, which opened its doors in 1934, was founded as a general hospital to welcome all patients, regardless of race, religion, language or ethnic background,” states Dr. Lawrence Rosenberg, President and CEO of the organization.
“The hospital was established in a less enlightened era, when Jewish doctors in Montreal could not find jobs due to prevailing prejudice. Similarly, Jewish patients could not be cared for in an environment that was sensitive to their unique cultural and religious needs.
“To emphasize the hospital’s opposition to discrimination of any type, it became the first healthcare institution in Quebec to officially designate itself as being ‘non-sectarian’ – that is, open to everyone (patients and employees alike), regardless of their background.”


JEWISH GENERAL HOSPITAL
The JGH is a tertiary-care academic medical center, one of McGill University’s flagship teaching hospitals. During its first 81 years, it functioned as an independent institution.
However, in 2015, as a result of a reorganization of Quebec’s public healthcare system, the hospital became the hub of a newly constituted Integrated Health and Social Services University Network for West-Central Montreal, commonly known as CIUSSS West-Central Montreal (“CIUSSS” is an abbreviation of the French term for the network).
CIUSSS facilities are located on 34 different sites in an area covering about 21 square miles. In addition to the JGH, this network includes six long-term care facilities, five community clinic/services organizations, 25 group medical practices, two rehabilitation hospitals and three rehab centers.
“Officially, the CIUSSS is responsible for providing services to a population of 380,091, with growth of 9.1 percent anticipated by 2036,” Dr. Rosenberg informs us. “In reality, we already serve well over 750,000 people, half of whom come from outside our territory. These users of the system span the entire age range, with 18 percent being 17 years old or below; 64 percent between the ages of 18 and 64; and 18 percent over 65.
“Interestingly, more than 42 percent of the people in our territory are immigrants, who represent 34 percent of the population of Montreal. This is truly the immigrant basin of Canada.”
The JGH is also home to the Segal Cancer Centre, a provincial referral center that has become one of Canada’s (and the world’s) most renowned facilities in the diagnosis and treatment of cancer. Of key importance is the Centre’s research and its many collaborative endeavors with cancer centers around the world. Especially noteworthy are efforts to develop novel approaches to personalized medicine that offer each patient the most effective targeted treatments for their particular form of the disease.
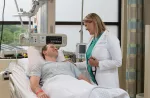
Also worth noting is the JGH’s in-depth and pace-setting expertise in geriatric medicine, developed through decades of treating a patient population which has consistently had a disproportionately high number of elderly individuals. This led to the launch in 2021 of the expanded Lieberman Family Wellness in Aging Geriatric Centre, whose aim is not only to treat illness, but to help each elderly person to maintain an optimum level of health and autonomy that is appropriate for their particular condition and circumstances.
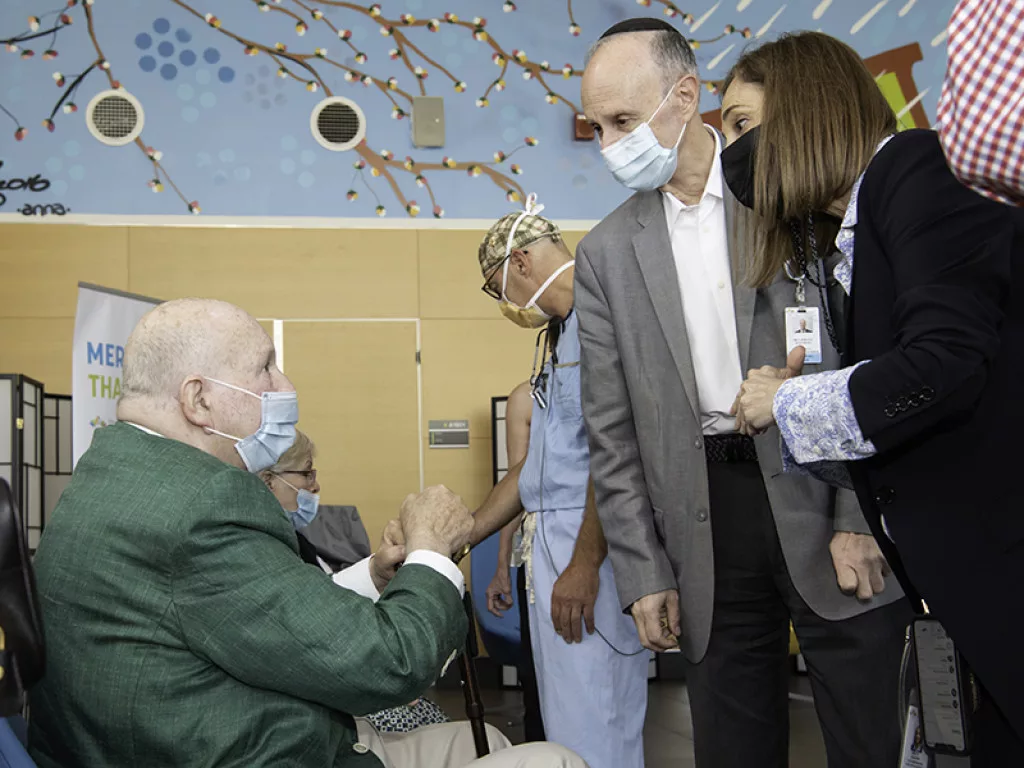
COMBATTING COVID-19
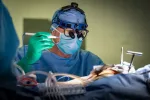
In the course of leading his organization, Dr. Rosenberg has seen it – and the broader sector – evolve during a unique period of enormous change and development, prompted largely by the COVID-19 pandemic. Since the JGH played a leading role in Quebec in treating infected patients, extensive preparation was required. Included was the development of protocols for the Emergency Department, Intensive Care, the medical units and the specialized areas, such as operating rooms, the cardiac catheterization laboratory and the various clinics.
“In addition, we have had to redefine patient pathways, including admission, transfers and discharges,” Dr. Rosenberg explains. “We have greatly increased extensive training in the use of personal protective equipment (PPE), with support from our Infection Prevention and Control team, so that we can function effectively in a pandemic environment.
“As the first wave of the pandemic rolled on, the hospital engaged in a very significant transfer of staff among our CIUSSS’s facilities, so that support could be provided to the COVID-19 units that had been set up.
“Telehealth, which had been in its preparatory stages before the pandemic struck – as part of the hospital’s very aggressive strategic plan for digital transformation – was rapidly rolled out to support patients and their families. Most of our ambulatory clinics established telehealth capabilities, and the cancer center, in particular, was able to maintain up to 85 percent of its usual activity through telehealth technologies.”
At the same time, the JGH established a digital command center to proactively manage beds and patient flow across the hospital and the rest of the CIUSSS. The command center was underpinned by artificial intelligence (AI) modelling, which permitted the JGH to predict COVID-19 hospitalizations one week in advance, with an outstanding accuracy rate of nearly 97 percent. As a result, the JGH was able to plan bed capacity and staffing, while ensuring an adequate supply of PPEs in the right places at the right time.

“The JGH was conceived by a group of visionary leaders in what was, and continues to be, among the most extraordinary Jewish communities in North America”
Dr. Lawrence Rosenberg, President and CEO, Jewish General Hospital
R&D
This type of support is intrinsic to the nature of the JGH as a medical institution, extending into the area of medical education and training, as well as research and development. The hospital’s principal R&D facility is the Lady Davis Institute for Medical Research (LDI), whose researchers have cross-appointments and strong connections to McGill University.
Since opening in 1967, the LDI has been at the forefront of health research, becoming one of the premier research institutes in Canada. “In the early 1980s, Dr. Mark Wainberg conducted pioneering work on the global HIV/AIDS pandemic, leading to the discovery of the anti-viral drug 3TC (Lamivudine) in 1989,” Dr. Rosenberg elaborates. “This drug is still used in combination with other medications to treat infections caused by HIV.
“During the COVID-19 pandemic, Dr. Brent Richards of the LDI has been prominent in gaining an understanding of the genetic risk for COVID-19 and establishing genetic predictors for the severity of the disease.
“As we emerge from this pandemic, the LDI will continue to expand its research focus on emerging infectious diseases, informed by our clinical experience at the JGH, one of the busiest infectious disease hospitals in Quebec and Canada.”
As well, the LDI has been at the forefront of mental health research, with Dr. Laurence Kirmayer’s pioneering achievements in cultural psychiatry, and Dr. Brett Thombs’ work in screening for depression in his international, collaborative DEPRESSED PROJECT. The continued focus on mental health is essential as society rebounds from the COVID-19 pandemic.
“The continued focus on mental health is essential as we rebound from the COVID-19 pandemic”
Dr. Lawrence Rosenberg, President and CEO, Jewish General Hospital

LDI’S EPIDEMIOLOGY CENTER
According to Dr. Rosenberg, the LDI’s Center for Clinical Epidemiology, led by Dr. Samy Suissa, plays a central role in assessing, monitoring and improving healthcare interventions. To do so, it relies on its leaders in pharmaco-epidemiology, which involves studying the risks and benefits of medications in the real-world conditions of clinical practice.
This has led to the development of new research and the extensive publication of articles about methods of accomplishing more rapid and accurate assessments of drug safety and effectiveness. Over the past 10 years, analysis of the data has been conducted by the Canadian Network for Observational Drug Effects Studies (CNODES), which is based at the LDI. CNODES includes a pan-Canadian team of scientists who draw on provincial healthcare databases to evaluate the effects of medications used by Canadians.
“This vision will now be expanded to include the development of our Centre for Digital Health and Applied Precision Medicine,” Dr. Rosenberg continues. “Its program will include the entire spectrum of research: basic research, including target identification and molecular pharmacology; prevention through the identification of disease-susceptibility genes and pathogenetic mechanisms; translational clinical research that specializes in clinical trials that incorporate correlation studies based on patient-derived bio specimens; and lastly, the identification of epidemiological and psychosocial contributors to health and illness.
“The focus will be on a bench-to-bedside-to-community approach. We aim to capture an Evolving Digital Patient Passport that will incorporate diverse datasets, including genomics data, epigenetic data, microbiome data combined with socio-economic data, clinical data and environment exposure data to personalize our approaches to human health and disease.”
This patient passport will evolve over time in the form of a “learning health journey”. With the changing demographics of Canada’s aging population, the JGH recognizes that most people will be living with multiple chronic diseases. Therefore, a focus on the early diagnosis of chronic diseases will be essential in improving the health of its patient populations.
“This will include an emphasis on innovative technologies, such as wearables and liquid biopsies,” Dr. Rosenberg says. “Can you imagine the day where an annual blood sample will be able to screen for early onset cancer, cardiovascular disease, and autoimmune diseases such as rheumatoid arthritis and diabetes? The change in focus to early diagnosis represents an inflection point that could change the course of the chronic disease trajectory and have major health benefits for society.”
HOSPITAL REBUILD – PHASE ONE
The JGH has also invested significantly in better patient care by building a new critical-care wing, known as Pavilion K, a project that has been implemented in three phases to date. The fourth and final phase, renovation of the legacy building, is soon to get under way. The Pavilion K project was named the 2017 PMI (Project Management Institute) Project of the Year (Elixir Competition).
Phase one was the launch of the new JGH Emergency Department (ED) in 2014. Between 2010 and 2014, the ED team pursued an innovative design that followed the adage, “form follows function”. Members of the team visited new EDs across Canada and the US, while contacting top ED architects and conceptual ED innovators in North America. A peripheral entry, linear pod design, was retained and married to the split-flow concept of ED patient flow.
“For many years, the JGH’s ED had been the busiest in Quebec,” Dr. Rosenberg tells us. “This occurred in the years that followed SARS and H1N1, and thus, preventive isolation issues remained at the forefront of the hospital’s concerns. This preoccupation resulted in a design consisting mostly of individualized patient examination rooms, with true ceilings, individualized ventilation and many negative pressure rooms in the pods. There was also a pressing need to manage the volume within the constraints of the designated space for the ED.
“Historically, the ED was an exceedingly noisy, stressful area where staff retention and the safe care of patients were preoccupying issues. This prompted us to implement an innovative design and use special materials to decrease the impact of noise. The ED became the first in Quebec to have a designated Rapid Assessment Zone (RAZ), the split-flow concept, peripheral entry for families, a linear pod design, and – somewhat presciently – an ED designed to handle a sudden influx of infectious patients in case of a pandemic crisis. Since then, these concepts have spread to the planning of other new EDs in Quebec. The JGH’s ED remains the busiest in the province, with close to 95,000 visits annually, prior to COVID-19.”
“Recruitment and employee well-being will also remain a key part of our focus moving forward, to ensure that members of our staff feel they are being well supported in the increasingly busy decade that lies ahead”
Dr. Lawrence Rosenberg, President and CEO, Jewish General Hospital
HOSPITAL REBUILD – PHASES TWO AND THREE
Phases two and three were designed to deliver on the promise of a “healing environment” on the nursing units and in all of the critical care areas, centered around the needs of patients and their families, and the requirements of medical professionals. Moreover, four clinical programs were completely reimagined to produce two units with integrated care trajectories based on the integrated practice unit (IPU) model. These were the Cardiovascular IPU (Cardiology, Cardiac Surgery, CVICU) and the Neurosciences IPU (co-localizing Neurology and Neurosurgery to provide an intermediate level of care, including a state-of-the-art rehabilitation room).
“A particularly noteworthy feature of the new pavilion resulted from intentional planning back in 2010: This was the design of a dedicated pandemic ward, the first of its kind for any new expansion project in a hospital in Quebec,” Dr. Rosenberg explains. “Our experience with H1N1 in 2009 raised questions about our preparedness for future pandemics. As a consequence, during the early design phase of Pavilion K, we incorporated a 24-bed unit, in which all rooms are single-bedded, equipped with negative pressure ventilation and including negative pressure antechambers.
“In addition, each nursing unit in Pavilion K is equipped with a certain number of negative pressure rooms – with and without antechambers – to accommodate additional patients requiring isolation. Accordingly, the JGH was designated as Montreal’s first adult COVID-19 site during the first wave of the pandemic, when as many as 176 COVID-19 patients were admitted at the peak.”
STERILIZATION AND SUSTAINABILITY
Pavilion K’s operating rooms (OR) were designed to prioritize strict infection control and to optimize the flows of patients and materials. The stand-out features include a direct link with sterilization (elevators for clean and soiled items); a sterile core, with automated dispensing cabinets; case cart trajectories; pre-and post-operative patient flows, previously mapped out using RFID; a dedicated robotic surgery theater, and a hybrid robotic room, enabling cardiac surgeons and cardiologists to work together concurrently.
“Special mention must also be made of the use of DMI machines in the sterile core,” Dr. Rosenberg adds. “These are automated dispensing machines, tracked by dedicated software in real time, that require no human interaction. Their installation has permitted us to have 100 percent control of ophthalmology lenses, including use by specific surgeons. This has enabled us to track the type of lens implanted into which patient, thereby reducing costs and theft.”
Furthermore, the Sterilization Department was renovated in 2016 and remains to this day a showcase of best practice for hospitals in Quebec. With Pavilion K, the JGH has been able to centralize all sterilization activities across its 34 sites. All of the norms of the Canadian Standards Association (CSA) are respected, and the JGH has had 100 percent compliance, as documented in four accreditations in a row.
“Lastly, we would like to draw attention to the important green issue of energy saving and sustainable development (ESSD),” Dr. Rosenberg says. “An $18.8 million ESSD project is now under way, with more than 85 percent of the measures completed. Ultimately, savings are estimated at $1.3 million per year. The project focuses on traditional energy management measures, but will also ensure the development of more ambitious and innovative measures, such as the installation of an aerothermal system to supplement the heating network of the JGH.”
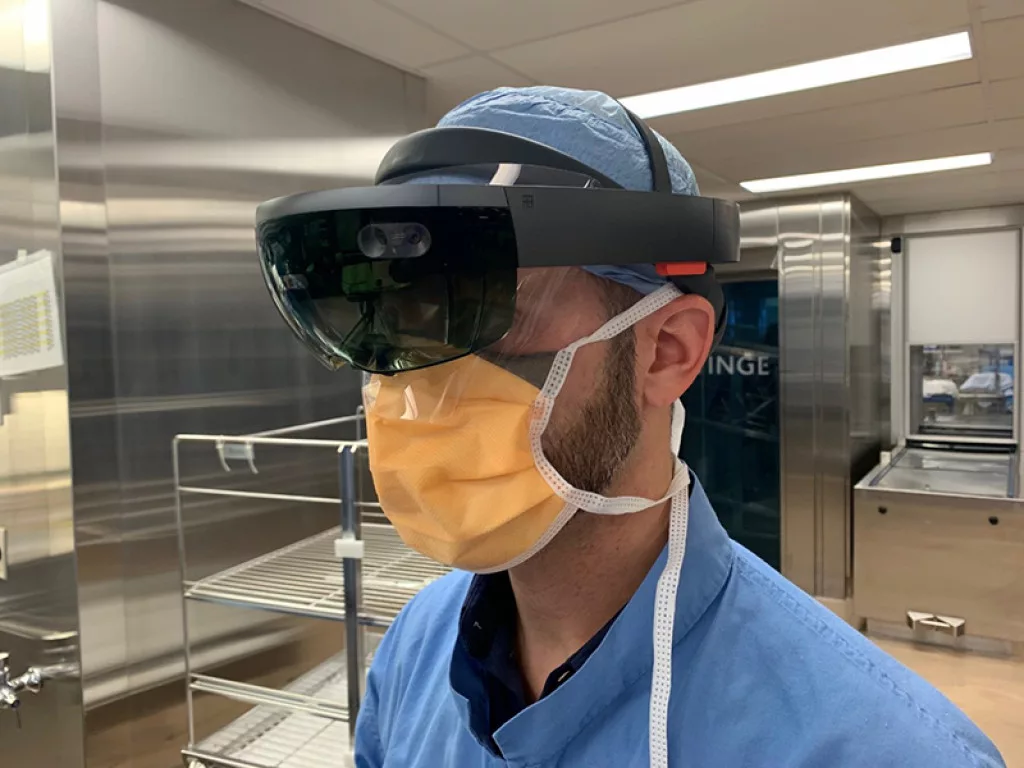
DIGITAL HEALTH
Looking forward, the JGH will continue to implement its digital health strategic plan, including its Connected Health Record, a next-generation electronic health record (EHR) under co-development; expanding data analytics and the data science portfolio with an international partner; introducing digital assistants – for example chatbots –to facilitate user interaction and experience.
“We will expand the operations of our command center to include AI-based modelling and data analysis,” Dr. Rosenberg notes. “Virtual care will also be a focal point of our future activities, and we will scale up our COVID@HOME program to a full HOSPITAL@HOME program.”
Of key importance is OROT (“illumination” in Hebrew), the CIUSSS’s connected health innovation hub which is based at the JGH. OROT is bringing together healthcare professionals and private-Healthcare entrepreneurs to better understand the needs of healthcare users, co-develop prototypes, and integrate and commercialize the next generation of digital innovation. In a broader sense, Dr. Rosenberg explains, OROT is challenging its participants to do nothing less than “re-imagine the future of healthcare networks,” but always with an eye toward human-centered design.
“Recruitment and employee well-being will remain a key part of our focus moving forward,” Dr. Rosenberg adds. “This will ensure that members of our staff feel they are being well supported in the increasingly busy decade that lies ahead.”